- 3 MIN READ
IV Dressing Types: Acrylic vs. Silicone
Intravenous (IV) therapy is a common medical procedure that involves inserting a thin tube into
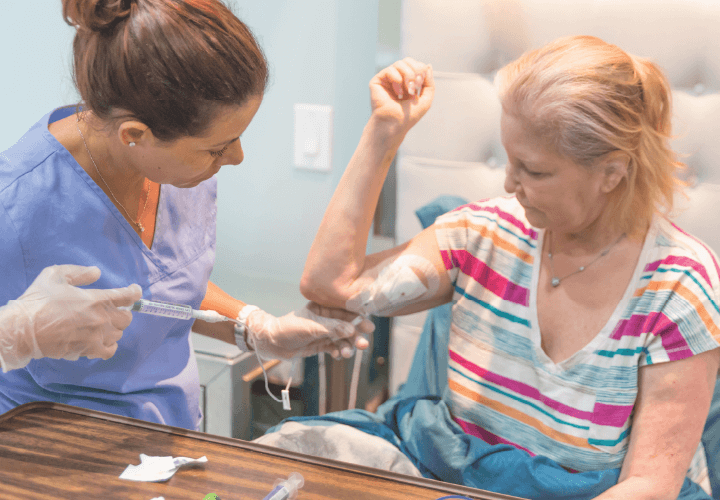
Share:
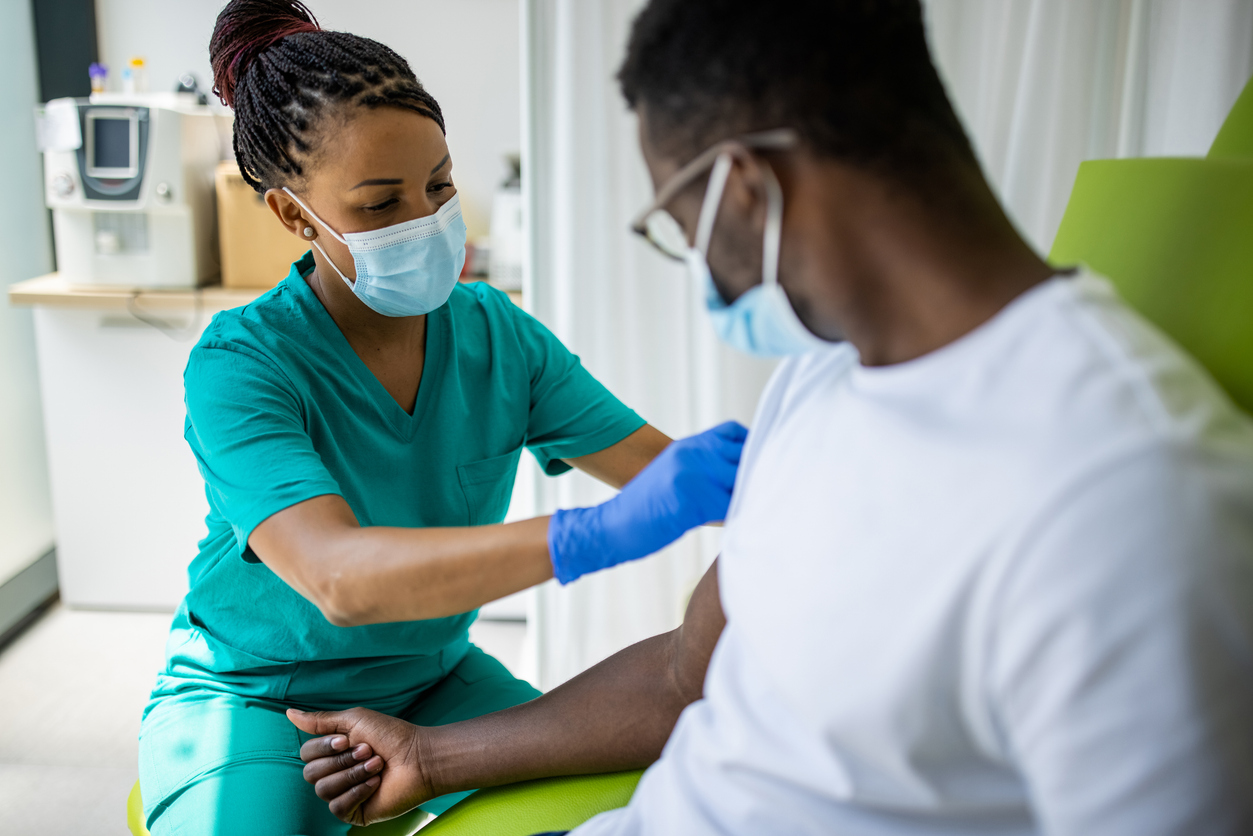
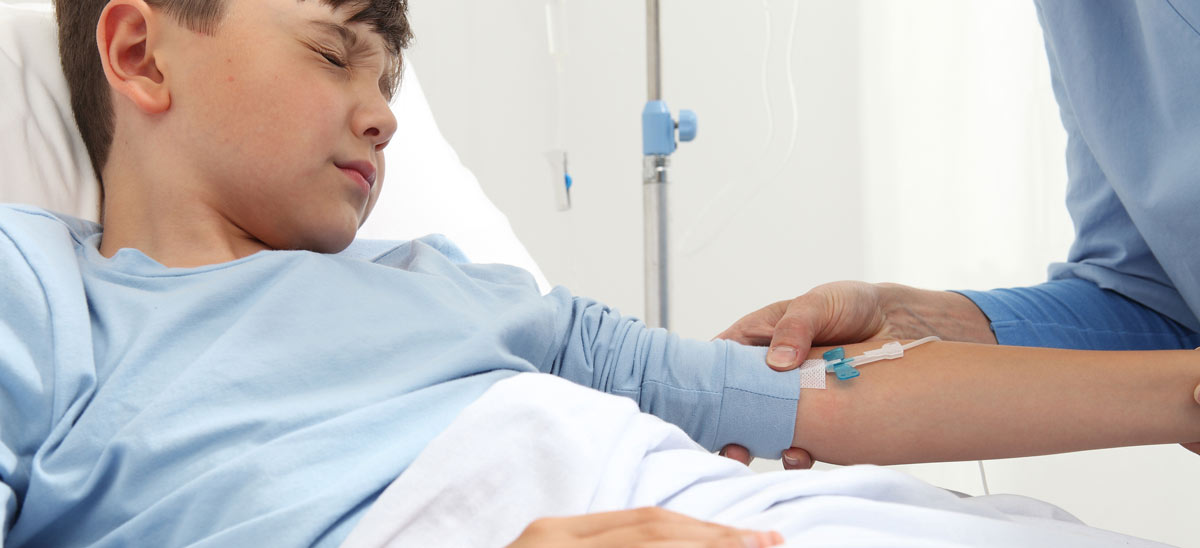
Intravenous (IV) therapy is a common medical procedure that involves inserting a thin tube into a vein to deliver fluids, medications, or blood products. While IV therapy is generally safe, it’s important to use the right materials and techniques to minimize the risk of complications. One crucial aspect of IV therapy is the choice of dressing used to secure the catheter to the skin.
What are IV Dressings?
IV dressings are specialized medical adhesive coverings that cover and protect the IV insertion site. They help to keep the catheter in place, prevent infection, and protect the skin from irritation.
The Function of IV Dressings
Ideal IV dressings should:
- Protect against infection: A dressing should create a barrier between the insertion site and external contaminants like bacteria and germs.
- Secure the catheter: The dressing should help keep the catheter in place to prevent dislodgement or movement, which can cause discomfort, pain, and increase the risk of further complications.
- Provide antimicrobial protection: Some dressings incorporate antimicrobial agents like chlorhexidine or silver to help prevent growth of microorganisms on the skin that can lead to infection.
- Allow for visibility: The dressing should be transparent to allow healthcare providers to easily monitor the insertion site for signs of infection or complications.
- Be comfortable: The dressing should be comfortable while the patient is wearing it and during removal.
- Protect skin integrity: The dressing should not damage or irritate the patient’s skin.
How are IV Dressings Designed
IV dressings are designed with several key features:
- Shape and size: The shape and size of the dressing will vary depending on the type and location of the IV insertion site.
- Adhesive properties: Dressings use different types of adhesives to adhere to the skin. The two most common types are acrylic and silicone adhesives.
- Breathability: The dressing should allow for air circulation to prevent moisture buildup and skin irritation.
- Barrier properties: The dressing should create an environmental barrier to prevent the entry of bacteria and other contaminants.
- Antimicrobial properties: Some dressings may contain antimicrobial agents to help prevent infection.
- Ease of application and removal: The dressing should be easy to apply and remove without causing discomfort or skin irritation.
Complications Associated with IV Therapy
Care should always be taken to prevent the complications which can arise during IV therapy, including:
- Dislodgement: The catheter may become dislodged if it is not adequately secured.
- Vessel wall trauma: Movement of the catheter can damage the blood vessel wall, leading to complications like thrombosis (blood clot formation).
- Extravasation: This occurs when medication or fluid leaks out of the vein into the surrounding tissues.
- Phlebitis: This is an inflammation of the vein that can cause pain, redness, and swelling.
- Medical Adhesive-Related Skin Injuries (MARSI): These injuries can occur when the adhesive used to secure the dressing irritates or damages the skin.
- Infection: Bacteria can enter the bloodstream through the IV site, leading to infection.
The Difference Between Acrylic vs. Silicone Dressings
The choice of adhesive is an important factor to consider when selecting an IV dressing. The two most common types of adhesives are acrylic and silicone.
Acrylic Adhesives
- Advantages:
- Strong and durable
- Relatively inexpensive
- Disadvantages:
- Can be harsh on the skin and cause irritation or skin tears upon removal
- May require the use of skin barriers and adhesive removers
Silicone Adhesives
- Advantages:
- Gentle on the skin
- Less likely to cause skin irritation or damage
- Easy to remove without the need for adhesive removers
- Disadvantages:
- May be more expensive than acrylic adhesives
- May require additional fixation for added security
Selecting the Right IV Dressing for the Patient
When selecting an IV dressing, it’s important to consider the individual needs of the patient. Factors to consider include:
- Skin condition: Patients with sensitive skin or a history of skin irritation may benefit from silicone dressings.
- Length of IV therapy: If the IV is expected to be in place for a long period, a gentle, skin-friendly dressing can help maintain skin integrity over the duration of therapy.
- Patient comfort: The dressing should be comfortable for the patient to wear and should not cause any discomfort or restriction of movement.
By carefully selecting the appropriate IV dressing, healthcare providers can help to minimize the risk of complications while improving patient comfort during IV therapy.
References
- Open Forum Infectious Diseases – Peripheral Intravenous Catheters
- Journal of Infusion Nursing – Improving Vascular Access Outcomes and Enhancing Practice
- International Wound Journal – Removal of adhesive wound dressing and its effects on the stratum corneum of the skin
- British Journal of Nursing – Preventing Medical Adhesive-Related Skin Injury (MARSI)
- NursingCenter – Complications of Peripheral I.V. Therapy
Covalon
If you are an individual reading this, please consult your health care provider before making any health care decisions, for guidance about a specific medical condition, and for use of any specific products. Covalon expressly disclaims responsibility and shall have no liability for any damages, loss, injury, or claim whatsoever suffered as a result of your reliance on any of the material or information contained in its blog articles or on the website
Related Blogs
Accurate wound measurement plays a vital role in wound care..
Getting an IV is a common and relatively minor medical..
The role of bedside nursing is becoming increasingly important as..